Bruxism is a repetitive jaw-muscle activity characterized by clenching or grinding of the teeth and/or thrusting of the mandible. It may occur during sleep or while awake and has a multifactorial aetiology involving biological, psychological, and lifestyle factors.
Reported prevalence varies widely in children, with many cases resolving naturally with age. While bruxism is often benign, it may be associated with tooth wear, temporomandibular discomfort, or underlying medical conditions.
Core principles include:
Management should be individualized, and in many cases active intervention may not be required.
Diagnosis of bruxism should include a thorough history, clinical examination, and possible assessment of muscle activity.
(Consensus-based recommendation; Global agreement: 98%)
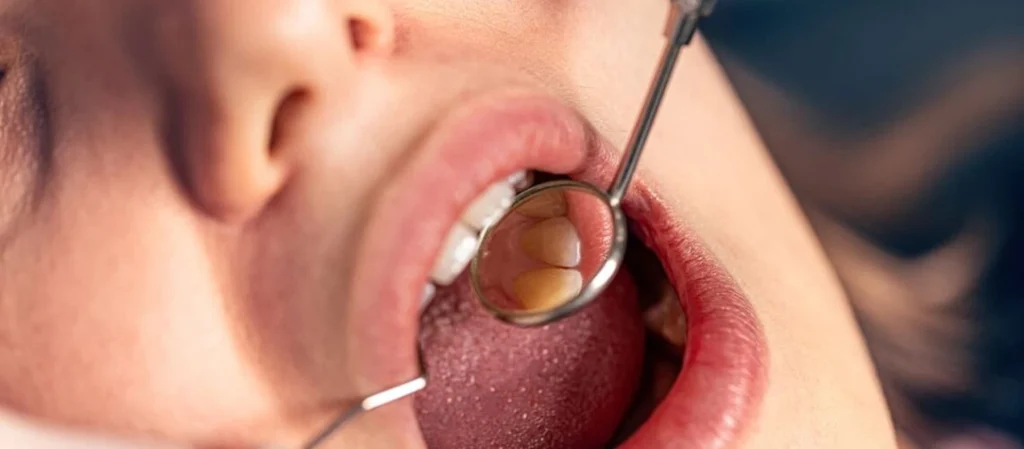
Minimum diagnostic criteria include reported tooth grinding or clenching together with abnormal tooth wear, bruxism-related sounds, or muscle discomfort.
(Consensus-based recommendation; Global agreement: 100%)
Assessment of possible gastro-oesophageal reflux disease should be considered when evaluating tooth wear that may be associated with bruxism.
(Consensus-based statement; Global agreement: 98%)
Clinical examination should include assessment of the muscles of mastication, temporomandibular joint function, mouth opening, and tooth wear patterns.
(Consensus-based recommendation; Global agreement: 96%)
Management should be individualized and may include behavioural strategies, occlusal splints, rapid palatal expansion, or monitoring without active treatment.
(Consensus-based recommendation; Global agreement: 93%)
Referral to a paediatrician or physician should be considered when bruxism may be related to systemic medical conditions.
(Consensus-based recommendation; Global agreement: 96%)
There is currently insufficient evidence to support pharmacological management of sleep bruxism in children.
(Consensus-based recommendation; Global agreement: 93%)
To support clinical implementation and knowledge translation, IAPD provides additional educational materials.
The IAPD podcast series explores evidence-based approaches to paediatric dental care and clinical decision-making.
Selected IAPD webinars address pain management strategies and clinical decision-making in paediatric dentistry.
International Association of Paediatric Dentistry (IAPD).
IAPD Foundational Articles and Recommendations on Behaviour Guidance in Paediatric Dental Patients.
Originally published 2019. Global Agreement Validation 2022.












| Cookie | Duration | Description |
|---|---|---|
| cookielawinfo-checkbox-analytics | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookie is used to store the user consent for the cookies in the category "Analytics". |
| cookielawinfo-checkbox-functional | 11 months | The cookie is set by GDPR cookie consent to record the user consent for the cookies in the category "Functional". |
| cookielawinfo-checkbox-necessary | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookies is used to store the user consent for the cookies in the category "Necessary". |
| cookielawinfo-checkbox-others | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookie is used to store the user consent for the cookies in the category "Other. |
| cookielawinfo-checkbox-performance | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookie is used to store the user consent for the cookies in the category "Performance". |
| viewed_cookie_policy | 11 months | The cookie is set by the GDPR Cookie Consent plugin and is used to store whether or not user has consented to the use of cookies. It does not store any personal data. |